Pressure Sore (Pressure Injury) Prevention Basics – What Works at Home?
If you care for someone with limited mobility, poor circulation, diabetes, or incontinence, skin care is not just an extra step—it is essential for their safety. Pressure sores, also known as pressure ulcers or injuries, develop when constant pressure or rubbing reduces blood flow to the skin and tissue. These sores usually appear over bony areas like the tailbone, heels, hips, ankles, elbows, and shoulder blades. Here are some tips to help you prevent pressure sores while caring for your loved one at home.
1) Know Who is at Higher Risk

A loved one is at higher risk when they have:
- Limited mobility (bedbound, wheelchair use, difficulty turning)
- Moisture exposure (incontinence, sweating, wound drainage)
- Poor nutrition/hydration or recent weight loss
- Reduced sensation (neuropathy, spinal cord injury)
- Poor circulation/diabetes, advanced age, fragile skin
Caregiver mindset: Prevention is a system— Positioning + Skin checks + Moisture control + Nutrition + The right surfaces. All of these aspects must be examined and correctly implemented to prevent pressure sore.
2) Daily Skin Checks: the “2-minute scan”
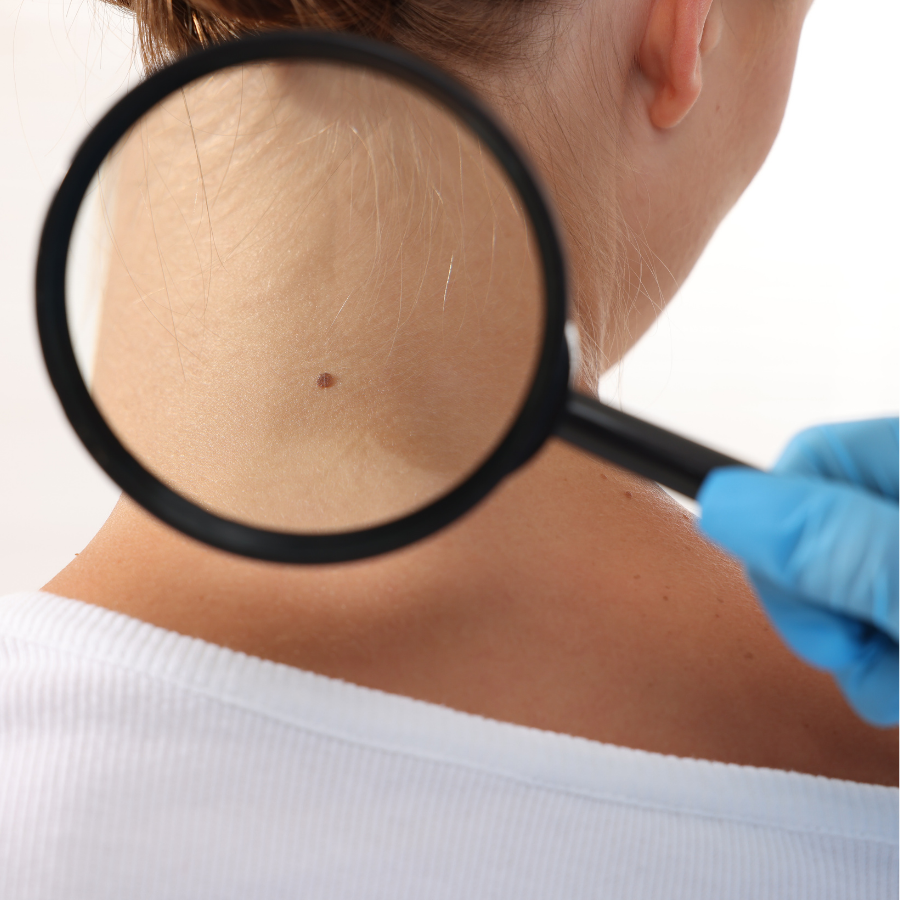
Once in the morning and once at bedtime (or at every brief change), check:
- Tailbone/sacrum, buttocks, hips
- Heels/ankles (heels are common and can worsen fast)
- Elbows, shoulder blades, back of the head
- Any area under tubing, braces, oxygen cannulas, or medical devices
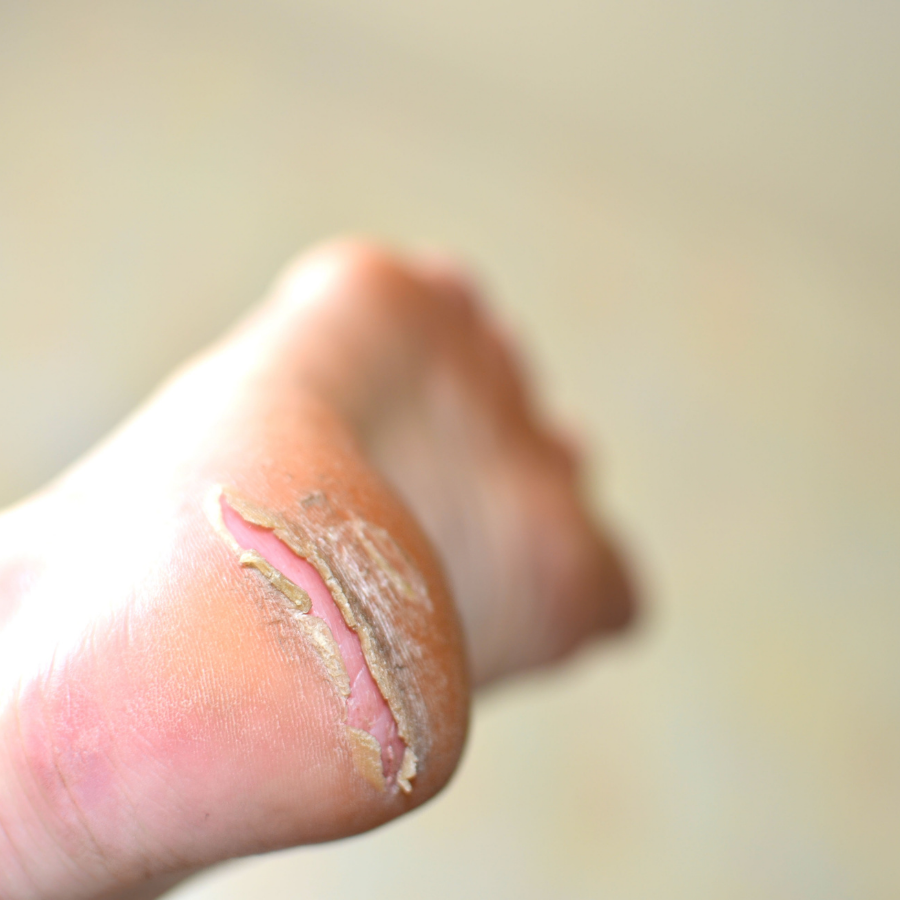
Early warning signs:
- Redness that doesn’t fade after 10–15 minutes off pressure
- Skin that feels warmer/cooler, firmer, spongy, or painful
- Blistering, purple/maroon discoloration, skin breakdown
If you notice a concerning spot, remove pressure from the area right away, protect it, and let the nurse or clinician know, especially if the skin is purple/maroon or skin is opening.
3) Repositioning and Offloading (Pressure Relief is Non-Negotiable)
Repositioning should be individualized (based on the person’s condition, tolerance, and support surface), but the home-care “default” is:
- Bedbound: change position at least every ~2 hours if tolerated
- Chair/wheelchair: shift weight every 15–30 minutes if possible; if not, assist to reposition at least hourly
Key technique: lift—don’t drag. Dragging causes shearing (skin layers sliding), which raises injury risk.
Heel protection: To protect the heels, place apillow under the calves so the heels are lifted off the bed, rather than placing a pillow directly under the heels. This keeps the heels from touching any surface all the time and helps prevent pressure injuries.
4) Moisture Management (Urine/Stool are Skin Irritants)
Moisture + pressure is a common pathway to skin breakdown. Practical basics:
- Clean promptly after incontinence episodes
- Use pH-balanced cleansers when available and avoid harsh scrubbing
- Pat dry, then apply a moisture barrier (cream/ointment) as advised
- Change wet briefs/pads quickly; avoid “layering” multiple pads that trap moisture and heat
5) Nutrition and Hydration Support Skin Integrity
Skin needs enough protein, calories, vitamins, minerals, and fluids to stay healthy and heal. Helping your loved one at mealtimes can help increase eating and drinking. If your loved one is not eating well, has wounds that heal slowly, or is losing weight, talk to their doctor about a nutrition plan or ask for a referral to a dietitian.

6) Support Surfaces Matter
If your loved one is high risk or already has a pressure injury, ask about:
- Pressure-redistributing mattress overlays or specialized mattresses
- Seat cushions designed for pressure redistribution (not donut cushions unless prescribed)

References
Agency for Healthcare Research and Quality. (2013). Pressure ulcer risk assessment and prevention: Comparative effectiveness (Comparative Effectiveness Review No. 87). https://effectivehealthcare.ahrq.gov/sites/default/files/pdf/pressure-ulcer-prevention_research.pdf
National Pressure Injury Advisory Panel. (n.d.). Prevention points. https://npiap.com/page/PreventionPoints
National Institute for Health and Care Excellence. (2014). Pressure ulcers: Prevention and management (NICE Guideline CG179). https://www.nice.org.uk/guidance/cg179

